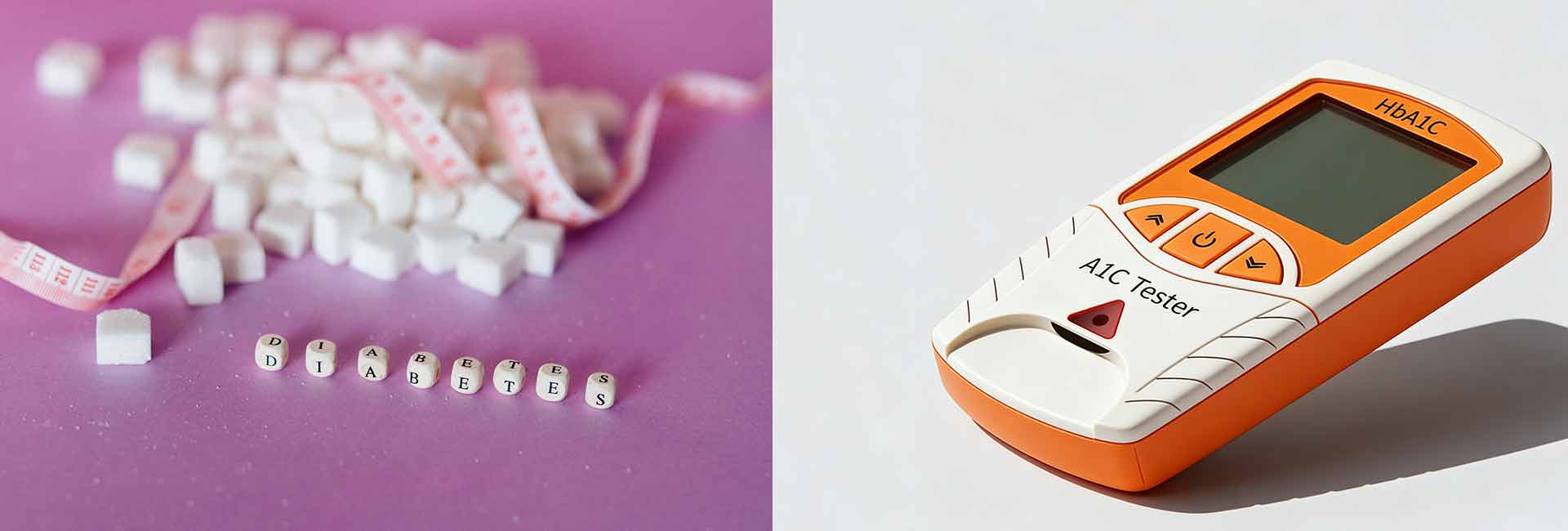Hemoglobin A1C measures the average blood sugar attached to hemoglobin over about three months. This test plays a key role in diabetes and prediabetes management because it helps identify people at risk and those who need treatment. About 21.4% of adults with diabetes remain unaware of their condition.
- A1C testing helps lower the risk of complications, such as nerve or kidney problems.
- Socioeconomic factors may affect access to care, but universal healthcare settings can reduce these barriers.
| Finding | Detail |
|---|---|
| A1C Cutoff for Undiagnosed Diabetes | 5.9% identifies subjects with undiagnosed diabetes |
| Prevalence of Microvascular Complications | Up to 25% of newly diagnosed patients had complications, indicating a lag in diagnosis |
Key Takeaways
- HbA1c measures average blood sugar over the past three months, helping identify diabetes and prediabetes.
- A1C testing lowers the risk of complications like nerve and kidney damage, promoting better health.
- Understanding A1C results empowers patients to make informed decisions about their diabetes management.
- Lifestyle changes, such as exercise and diet, can significantly improve A1C levels and overall health.
- Consult your doctor if your A1C is 6.5% or higher to ensure effective management and prevent complications.
What Is Hemoglobin A1C?
HbA1C Explained
Hemoglobin A1C serves as a key marker for long-term glucose control in diabetes. This molecule forms when glucose in the bloodstream binds irreversibly to hemoglobin in red blood cells. The process begins when glucose attaches to the NH2-terminal valine on the beta chain of hemoglobin, creating an unstable Schiff base. This base then undergoes a chemical change, resulting in a stable glycated hemoglobin molecule. Once glucose binds, it remains attached for the lifespan of the red blood cell, which is about 120 days.
- Hemoglobin A1C is a standard test for measuring glycated hemoglobin.
- HbA1c test provides a reliable indicator of average blood sugar over the previous three months.
- Healthcare providers use this test to assess the risk of diabetes-related complications and to evaluate glycemic control.
Note: Many people with diabetes do not fully understand what the A1C test measures. Studies show that nearly half of individuals with diabetes cannot explain the purpose of this test.
How It Reflects Average Blood Sugar?
The A1C test measures the percentage of hemoglobin molecules in the blood that have glucose attached. As blood sugar levels rise, more glucose binds to hemoglobin. Because red blood cells live for about 120 days, the test reflects average blood sugar during the past two to three months. The results appear as a percentage. Higher percentages indicate higher average blood sugar levels. Healthcare providers sometimes convert a1c results to estimated average glucose (eAG) values, making it easier for patients to understand their results in familiar units.
Difference from Daily Blood Sugar Checks
| Aspect | Hemoglobin A1C Testing | Daily Blood Glucose Monitoring (CGM) |
|---|---|---|
| Purpose | Assesses average blood glucose over the past 2-3 months | Provides real-time glucose levels for immediate management |
| Accuracy | Gold standard for long-term glycemic control | Offers continuous monitoring but may vary due to factors |
| Measurement Frequency | Typically done every 3 months | Continuous, every 1-5 minutes |
| Factors Affecting Results | Influenced by RBC turnover, anemia, and other conditions | Real-time data can be affected by food intake and activity |
| Clinical Use | Evaluates overall diabetes management effectiveness | Helps in daily management and immediate decision-making |
A1C testing gives a big-picture view of glucose control, while daily monitoring helps with immediate decisions. Both tools play important roles in diabetes management, but they serve different purposes.
Importance of Hemoglobin A1C
Role in Diabetes Diagnosis
Hemoglobin A1C plays a central role in diagnosing diabetes and prediabetes. Healthcare providers use this test to identify individuals at risk and to confirm a diagnosis. The American Diabetes Association (ADA) sets clear thresholds for interpretation. An A1C value of 5.7% to 6.4% signals prediabetes, while a value of 6.5% or higher confirms diabetes. These thresholds help clinicians make timely decisions and start interventions early.
| Condition | A1C Threshold | Sensitivity | Specificity |
|---|---|---|---|
| Prediabetes | 5.5% | 68.5% | 61.4% |
| Diabetes | 6.1% | 81.8% | 98.8% |
| ADA Thresholds | 5.7% – 6.4% | 31.6% | N/A |
| ≥6.5% | 63.6% | N/A |
Clinicians often compare hemoglobin A1C with other diagnostic tools. Fasting plasma glucose (FPG) and oral glucose tolerance tests (OGTT) also help diagnose diabetes. However, a1c offers a practical advantage because it does not require fasting. The following table shows how these tests compare:
| Test Type | Sensitivity | Specificity |
|---|---|---|
| HbA1c | 50% | Lower than FPG |
| FPG | 17% | 97% |
| OGTT | 18% (DM) | 59% (Prediabetes) |
International guidelines sometimes differ. For example, some recommend a screening cut-point of 6.0% for close follow-up. The diagnostic cut-point often remains at 6.5%, supported by glucose tests. These variations reflect ongoing research and regional practices.
Monitoring Long-Term Glucose Control
Doctors rely on A1C to monitor long-term glucose control in people with diabetes. This test provides a snapshot of average blood sugar over several months. Regular monitoring helps track progress and adjust treatment plans. Studies show that the introduction of continuous glucose monitoring (CGM) can lower mean A1C levels from 8.2% to 7.1%. This significant decrease demonstrates the value of A1C as a reliable measure for diabetes management.
Tip: Patients who monitor their A1C regularly can work with their healthcare team to make informed decisions about medication, diet, and lifestyle.
International organizations set different targets for A1C. The ADA has lowered its recommended targets, while the International Society for Pediatric and Adolescent Diabetes suggests a goal below 7.5%. The American College of Physicians sometimes recommends higher targets, which has sparked debate among experts. These differences highlight the importance of individualized care.
Preventing Complications

Maintaining A1C levels reduces the risk of serious complications. High A1C values indicate poor blood sugar control, which damages small blood vessels. This damage affects nerves, kidneys, and eyes. Nerve damage, or neuropathy, develops when high blood sugar harms the vessels that nourish nerves. Symptoms include tingling, numbness, and pain. Keeping A1C within target ranges helps prevent or slow the progression of neuropathy.
- Diabetic retinopathy, a leading cause of blindness, results from high A1C damaging retinal blood vessels. This can cause leakage, blurred vision, and severe vision loss.
- High A1C also increases the risk for cataracts and glaucoma, further threatening eye health.
- Controlling A1C reduces damage to blood vessels critical for nerve, kidney, and vision function, lowering the risk of complications.
Doctors emphasize the importance of A1C testing for all people with diabetes. Early detection and consistent management protect long-term health and quality of life.
A1C Test & Results
How the A1C Test Works?
The A1C test measures the percentage of hemoglobin molecules with glucose attached, reflecting average blood sugar levels over two to three months. Healthcare providers recommend A1C testing every three to six months for adults with diabetes, depending on their control. Most individuals should have the A1C test at least twice a year, with more frequent testing if their management plan changes. Regular monitoring helps doctors adjust medications and dietary recommendations, improving quality of life and reducing healthcare costs.
- Individuals with diabetes should have their A1C test every 3 to 6 months.
- Most people with diabetes need A1C testing at least twice a year.
Routine screening before certain surgeries, such as hip arthroplasty, can save costs and prevent complications. Point-of-care A1C testing improves access for underserved populations.
Using an A1C Tester
Patients can choose A1C tester. A1C test kit provides laboratory-quality results and include lancets, collection devices, and instructions for accurate sample collection. Testing methods include point-of-care devices for immediate results and mail-in services for laboratory analysis. Studies show that 93.2% of A1C values from lay users fall within ±13.5% of laboratory reference values, demonstrating high accuracy. A1C tester features automated chemistry and error-correcting software, ensuring precision and ease of use.
| Testing Method | Accuracy | Notes |
|---|---|---|
| Lab-blotter | High | Preferred by most patients; widely supported in practice |
| Routine Venous | Moderate | Standard method for A1C measurement |
| Home-blotter | Viable | Good for those with limited access; reasonable alternative |
Note: Hemoglobin variants or anemia can affect A1C test results. Any condition that shortens red blood cell survival may falsely lower A1C values.
Interpreting A1C Levels
Doctors use A1C test results to assess diabetes control and risk of complications. The following table shows what different A1C percentages mean:
| Diagnosis | A1C Level |
|---|---|
| Normal | below 5.7 percent |
| Prediabetes | 5.7 to 6.4 percent |
| Diabetes | 6.5 percent or above |
An A1C level below 5.7 percent is considered normal. Levels between 5.7 and 6.4 percent indicate prediabetes, which increases the risk for type 2 diabetes. An A1C of 6.5 percent or above confirms diabetes. Maintaining an A1C level under 7 percent lowers the risk of diabetes-related complications. Doctors recommend combining A1C testing with continuous glucose monitoring for a comprehensive view of blood sugar management.
Managing A1C Levels
Target A1C Goals
Major diabetes organizations recommend different a1c goals based on individual needs. The American Diabetes Association suggests a target A1C goal of less than 7% for many nonpregnant adults who do not experience significant hypoglycemia. Lower A1C levels may be suitable for some people if they can achieve them safely. Less strict a1c goals, such as below 8%, may fit those with limited life expectancy or when treatment risks outweigh benefits. The American College of Physicians advises that for patients with a life expectancy under 10 years, especially those over 80 or with chronic illnesses, the focus should shift to minimizing symptoms rather than strictly controlling a1c. Age, ethnicity, and comorbid conditions also influence a1c target levels. Younger patients, especially non-Hispanic Black and Hispanic individuals, often require more stringent a1c goals due to earlier diagnosis and fewer comorbidities.
Individualized A1C goals help address unique health needs and improve diabetes management.
Lifestyle and Medication Tips
Lifestyle changes play a major role in reaching A1C goals. Regular exercise, such as running, can lower A1C levels. Research shows that runners have an average a1c of 7.31 compared to 7.98 in non-runners. Dietary adjustments also help. A low-carbohydrate diet can reduce a1c by 0.23%, along with improvements in body weight and waist circumference. Support groups and diabetes education programs provide additional benefits. Structured virtual education, smartphone applications, or a combination of both can lead to lasting reductions in a1c results.
| Group | Average HbA1c Level |
|---|---|
| Runners | 7.31 |
| Non-Runners | 7.98 |
| Intervention Type | Description | Outcome |
|---|---|---|
| Virtual Education | 6–8 hours with counseling | Reduced A1C values |
| Smartphone App | Self-paced learning | Reduced A1C values |
When to Consult Your Doctor?
People with diabetes should consult a healthcare provider if their A1C is 6.5% or higher. Medical advice is important if symptoms of high blood sugar appear. Severe symptoms, such as chest pain, confusion, or shortness of breath, require urgent care. The a1c test helps track progress, but regular communication with a doctor ensures safe and effective management.
Early intervention can prevent complications and support better long-term outcomes.
Conclusion

Hemoglobin A1C remains a cornerstone in diabetes management. Regular A1C testing helps individuals and healthcare providers track progress and adjust treatment. Patient education leads to better outcomes:
- Educational programs lower HbA1c levels in people with type 2 diabetes.
- Health literacy interventions improve both glycemic control and diabetes knowledge.
- Studies show a decrease in HbA1c from 8.17% to 7.44% after targeted education.
People benefit from using A1C tester,A1C test kit and seeking medical guidance. Proactive management supports long-term health and reduces complications.
FAQ
What Does an A1C Test Measure?
The A1C test measures the percentage of hemoglobin in red blood cells that has glucose attached. This value shows the average blood sugar level over the past two to three months.
How Often Should Someone with Diabetes Check Their A1C?
Doctors recommend checking A1C every three to six months. People with stable blood sugar may test less often, while those changing treatment plans may need more frequent checks.
Can Illness or Anemia Affect A1C Results?
Yes. Illnesses that change red blood cell lifespan, such as anemia, can affect A1C accuracy. Results may appear falsely high or low. Doctors may use other tests if they suspect inaccurate readings.
Is It Possible to Lower A1C Quickly?
A1C reflects long-term blood sugar. Quick changes in daily glucose do not immediately lower A1C. Consistent healthy habits, such as exercise and diet, help reduce A1C over several months.
What Is the Difference Between A1C and Estimated Average Glucose (eAG)?
A1C shows a percentage, while eAG translates this value into an average blood sugar number (mg/dL). This conversion helps patients understand their results in familiar terms.